Tagged: 2.62

Blood part 2 White Blood Cells – Grade 9 Understanding for GCSE Biology 2.59 2.62 2.63B
The previous post looked at the structure and function of red blood cells and plasma. Now it is time to turn our attention to the rather more complex topic of white blood cells….. This is a topic in which the complexity can put people off but I am deliberately going to keep things simple (I hope!). If you are thinking about revision for GCSE, don’t worry about anything more complicated than in this post.
There are many types of white blood cell found in blood. But let’s keep things simple…. You need to understand the role of lymphocytes and phagocytes in defending the body against pathogens.
A pathogen is defined as “a microorganism that can cause a disease” and pathogens may be bacteria, viruses, protistans or fungi. Can you give me an example of an infectious disease caused by each class of pathogen?
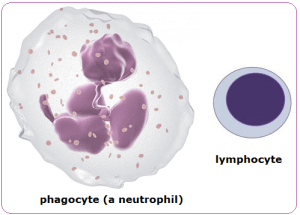
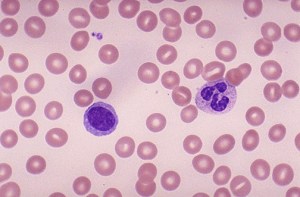
The structure of these two classes of white blood cell is important. The commonest phagocytes in blood are called neutrophils and they are easily recognised by their irregular shaped nucleus and cytoplasm packed full of granules. Lymphocytes are much smaller white cells and are identifiable by their clear cytoplasm and large spherical nucleus that takes up 90% of the volume of the cell.
So now we should look at how these two types of white blood cells defend the body against pathogens. Remember that the account on this post is an over-simplification of what is in reality an extremely complex process.
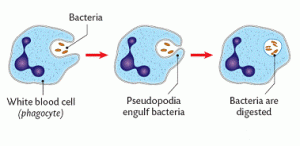
Let’s start with a phagocyte. These large cells are able to engulf invading pathogens in the blood and tissue fluid by a process called phagocytosis.
The phagocyte pushes out projections of its cytoplasm around the clump of bacteria. These projections are called pseudopodia and when they meet, the cell membrane of the phagocyte fuses together leaving the bacteria enclosed in a tiny membrane packet called a vesicle inside the cytoplasm. The phagocyte then fuses other vesicles that contain powerful digestive enzymes with the vesicle with the bacteria in, leading to the death and destruction of the bacteria. Simple.
The problem for phagocytes is this: how do they know what to engulf and destroy? This is where lymphocytes come in. One class of lymphocyte is able to secrete small soluble proteins called antibodies into the blood. Antibodies are specific to a particular surface marker on the invading pathogen and bind to it because the shape of the antibody and the shape of the surface marker are complimentary.
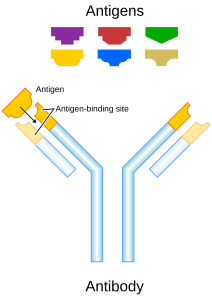
Now people always get confused between antibodies (the small soluble Y-shaped proteins secreted by lymphocytes) and antigens (the surface markers on the invading pathogen). Make sure you are completely clear on the difference in meaning of these two words….
 This diagram shows antibodies (green) binding to surface markers (antigens) on a bacterial cell.
This diagram shows antibodies (green) binding to surface markers (antigens) on a bacterial cell.
Antibodies produced by lymphocytes will coat the invading pathogen by binding to antigens on its surface. One effect of this is that phagocytes are stimulated to engulf the antibody-coated organism.
There are many different types of lymphocyte and not all can produce antibodies. Another important function of lymphocytes is to kill your own body cells when they are corrupted, either by the presence of a virus or by becoming cancerous.
Finally, can I draw your attention to two previous posts linked to this one. The first is on the role of platelets in blood clotting, the second on the difficult topic of immunity and how lymphocytes are responsible for giving you lifelong protection against certain infectious diseases.
https://pmgbiology.wordpress.com/2014/04/07/immunity-a-understanding-for-biology-igcse/
As always, please ask me questions either via the comment section below the post or with a tweet…. I will do my best to respond to any questions from anyone who is bothered to read my posts!
Platelets and Blood Clotting – Grade 9 Understanding for iGCSE Biology 2.64B
There is a specification bullet point in bold (paper 2 only) about blood clotting and the role of platelets, and students are sometimes not sure to what level of detail is needed for a full GCSE understanding of this topic. Well the good news is that the only questions I can recall are very straightforward indeed. But in this post I will give you a little more detail than the minimum needed for A* answers so that you can be confident you are completely clear on this part of the specification.
Why does blood need to clot?
Capillaries have a very thin wall (one cell thick in fact) so can easily tear and get damaged. This means that damage causes blood to leak into tissues forming a bruise and if the skin is broken, blood can be lost from the body entirely. Blood clotting is the response in the blood that ensures that blood loss is minimised and also that the time micro-organisms have to get into the blood stream is kept as short as possible. The surface of the skin is covered with millions of pathogenic organisms (mostly bacteria) all waiting for the chance to get into the blood stream through a cut or tear.
What are platelets?
Platelets are small fragments of cells found in bone marrow that then get into the blood and are carried round in the plasma. They are not entire cells as they lack a nucleus but they do play an essential role in blood clotting.
How does blood clotting work?
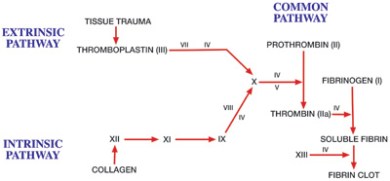
When the lining of a capillary is broken, platelets initially stick to the site of damage. They then trigger a series of reactions in the blood plasma that causes a clot to form. The details of how this works are too complicated to go into here but the basic idea is that in the blood plasma are a whole family of proteins called clotting factors. There is a cascade of reactions such that one clotting factor is activated and in turn, activates the next in the sequence. The final reaction in the clotting cascade is that a soluble protein called fibrinogen is converted into an insoluble fibrous protein called fibrin. Fibrin forms a mesh around the platelet cap covering the site of damage and this mesh traps red blood cells forming the final clot.
The roman numerals on the diagram above refer to clotting factors and each in turn is activated. You can see the final stage of the cascade is that soluble fibrin is converted into the fibrin clot.
Many of you will know of the disease where blood doesn’t clot called haemophilia. The commonest type of haemophilia is a genetic disease where patients cannot produce clotting factor VIII. This means one step in the clotting cascade does not work and so the blood cannot clot normally.
(Extension idea: find out the link between Haemophilia, the British Royal family and the 20th century history of Russia)